|
Key Takeaways:
|
Glaucoma symptoms can be easy to miss at first, which is why it’s called the “silent thief of sight.” Over time, rising eye pressure can damage the optic nerve, causing permanent vision loss if not treated. This guide explains the early signs, who’s at higher risk, and simple steps to prevent damage and protect your sight.
What is Glaucoma?
Glaucoma is a group of eye diseases that damage the optic nerve, the cable that carries images from the eye to the brain. The most common driver is higher-than-healthy eye pressure (IOP), but some people develop glaucoma even with “normal” pressure. Because early damage is usually silent, many people feel fine while slow vision loss is building.
Common types of Glucoma include:
- Open-angle glaucoma: The most common type, characterized by slow and progressive vision loss.
- Angle-closure glaucoma: A more severe form that occurs suddenly and requires immediate medical attention.
- Normal-tension glaucoma: Occurs despite normal eye pressure levels, making it difficult to detect early.
- Congenital glaucoma: Present at birth due to abnormal eye development.
Knowing the type helps your doctor choose the right tests and treatment.
Causes of Glaucoma
Glaucoma starts when the eye’s clear fluid (aqueous humour) doesn’t drain properly, so pressure strains the optic nerve or when the nerve is unusually sensitive to normal pressure.
- Blocked or inefficient drainage in the angle of the eye
- Genetics/family tendency affecting drainage or nerve health
- Eye injury or prior surgery that changes fluid outflow
- Health conditions that affect blood flow to the nerve (e.g., diabetes, high BP)
- Steroid medicines (drops, inhalers, tablets, skin creams) that can raise IOP
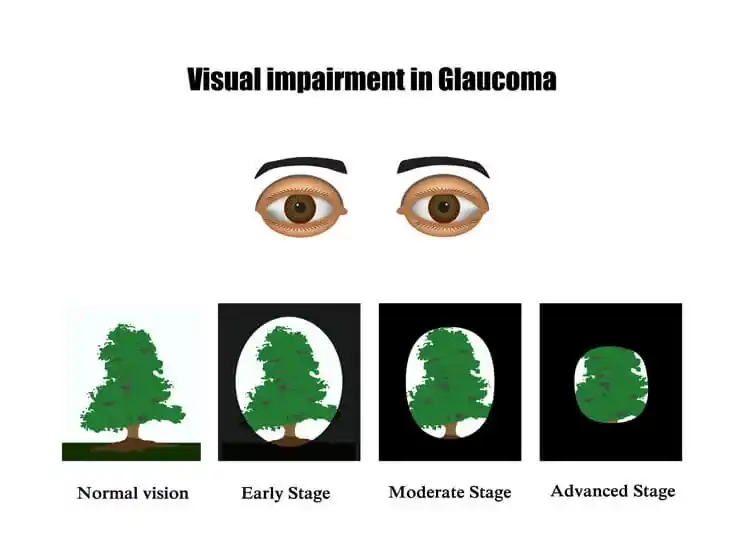
Why Symptoms Matter (The Silent Early Stage)?
Early glaucoma usually has no symptoms. Side-vision thins slowly, and the brain adapts, so people don’t notice until the disease is advanced. That’s why regular exams and pressure/nerve checks are essential, catching change early protects sight.
Who is at Risk?
Some people need closer and earlier testing because their risk is higher.
- Family history of glaucoma (parent or sibling)
- Age over 40 (risk rises with age)
- Thin corneas, high myopia, or past eye injury/surgery
- Diabetes, hypertension, sleep apnea, migraine/vascular issues
- Long-term steroid use (any form)
- Ethnicity: African, Hispanic, or Asian ancestry have higher risk in many studies
|
Note: Long screen time mainly causes dryness and eye strain. It doesn’t directly cause glaucoma, but poor posture, breath-holding during effort, or prolonged head-down positions can nudge pressure temporarily. Regular breaks and good posture are still smart habits. |
Main Symptoms of Glaucoma
Glaucoma begins quietly. Vision feels normal because the brain fills in missing pieces, and there’s no pain in most early cases. Over months and years, tiny gaps grow at the edges of sight, night lights start to glare, and tasks that were effortless begin to feel tiring.
Early, hard-to-notice signs (the “silent” stage):
- Side-vision slips first. You clip doorframes, miss steps on stairs, or not notice someone approaching from the side.
- Dim places feel tougher. Night driving needs extra effort; bright lights leave lingering halos.
- Things look a little washed out. Contrast fades, so grey text on a grey background is harder to read.
- Tired eyes after long tasks. Reading, spreadsheets, or phone scrolling bring on eye strain or a mild headache.
How it shows up in daily life:
- You need more light to read menus or medicine labels.
- You turn your head more to check mirrors or find items on shelves.
- New glasses help only a little, and the improvement doesn’t last.
Signs as disease advances:
- Patchy blind spots join together, creating tunnel vision, the centre is okay, but the world narrows.
- Persistent blur that doesn’t clear with blinking or a new prescription.
- Trouble judging steps, curbs, and edges, leading to stumbles or near-falls.
Emergency symptoms:
- Severe eye pain with redness and a sudden drop in vision.
- Halos around lights plus headache, nausea, or vomiting.
- This needs same-day medical care to protect sight.
Symptoms that can confuse you:
- Dryness, burning, or irritation are common in many eye problems and do not prove glaucoma.
- Frequent prescription changes alone aren’t a sure sign; glaucoma is confirmed by tests: eye pressure (IOP), optic nerve exam, OCT scans, and visual field maps.
Prevention & Eye Health
You can’t always prevent glaucoma, but you can lower glaucoma risk and protect your sight with steady habits and regular checks. Think of it as keeping the eye’s “pressure system” comfortable while caring for the optic nerve.
Smart daily habits:
- Move most days: Walking, cycling, or swimming helps overall blood flow and can support healthier pressure patterns.
- Sleep slightly head-up: Use an extra pillow or wedge to avoid night-time pressure rise.
- Sip water steadily: Small, regular sips are better than chugging large amounts at once.
- Go easy on caffeine and heavy straining: Multiple strong coffees/energy drinks, tight collars, or breath-holding lifts can nudge IOP up briefly.
- Protect your eyes: Wear safety eyewear for sports, DIY, and dusty work to avoid injury-related problems.
Screen time & comfort:
- Screens don’t cause glaucoma, but dryness and strain add discomfort.
- Follow 20-20-20 (every 20 minutes, look 20 feet away for 20 seconds), blink fully, and use adequate lighting.
- Artificial tears can help if your doctor approves.
Health conditions & medicines:
- Control blood pressure and diabetes per your physician’s plan.
- Tell your doctor about any steroid use (drops, inhalers, tablets, skin creams) since steroids can raise eye pressure.
- If you snore loudly or feel very sleepy during the day, ask about sleep apnea, which may affect optic nerve health.
“Eye exercises”: what helps (and what doesn’t)
- Relaxation routines like palming, gentle blinking, and look-away breaks can help with fatigue and dryness.
- These do not lower eye pressure or treat glaucoma; they’re for comfort only.
Check-ups are very important:
- Get regular eye exams with pressure checks, optic nerve evaluation, and (when advised) tests like OCT and visual fields.
- Especially if you’re over 40, have a family history, high myopia, thin corneas, diabetes, hypertension, or long-term steroid use.
When to Seek Urgent Care?
Some Glaucoma symptoms can’t wait.
Get same-day medical care if you have severe eye pain, sudden redness, a quick drop in vision, or halos with headache, nausea, or vomiting, these can be signs of an angle-closure attack. Also act fast if one eye suddenly goes blurry while the other seems fine, or if you notice many new floaters and flashes.
Conclusion
Glaucoma starts quietly, so symptoms can be easy to miss until damage has already begun. Knowing the early signs of glaucoma and your personal risk helps you act before vision is harmed. With regular check-ups and timely treatment, most people can slow or stop further loss and keep daily life clear and safe.
FAQs
What are early signs of glaucoma?
The early signs of glaucoma are side-vision loss, increasing night glare or halos, and needing more light to read, most of the time without pain.
Can glaucoma cause sudden vision loss?
Yes, glaucoma can cause sudden vision loss during an angle-closure attack, which is an emergency and needs same-day care.
Are symptoms of glaucoma different in men and women?
No, the symptoms of glaucoma are not different in men and women; symptoms are similar; differences are more about risk factors (age, hormones, health conditions) than the way symptoms feel.
Do young adults experience different glaucoma symptoms?
No, young adults do not experience different glaucoma symptoms; symptoms are largely the same, but young adults with high myopia or a strong family history should be checked earlier.
When should I see a doctor for glaucoma symptoms?
You should see a doctor for glaucoma symptoms promptly if side-vision feels unreliable, night glare is growing, new glasses don’t really help, or any sudden pain/redness or rapid blur appears.