|
Key Takeaways:
|
In this simple guide, we’ll explain the cortical cataract meaning, its causes, stages, grading, diagnosis and treatment options, so you know when to watch, when to act, and what to expect from surgery if you ever need it.
What is Cortical Cataract?
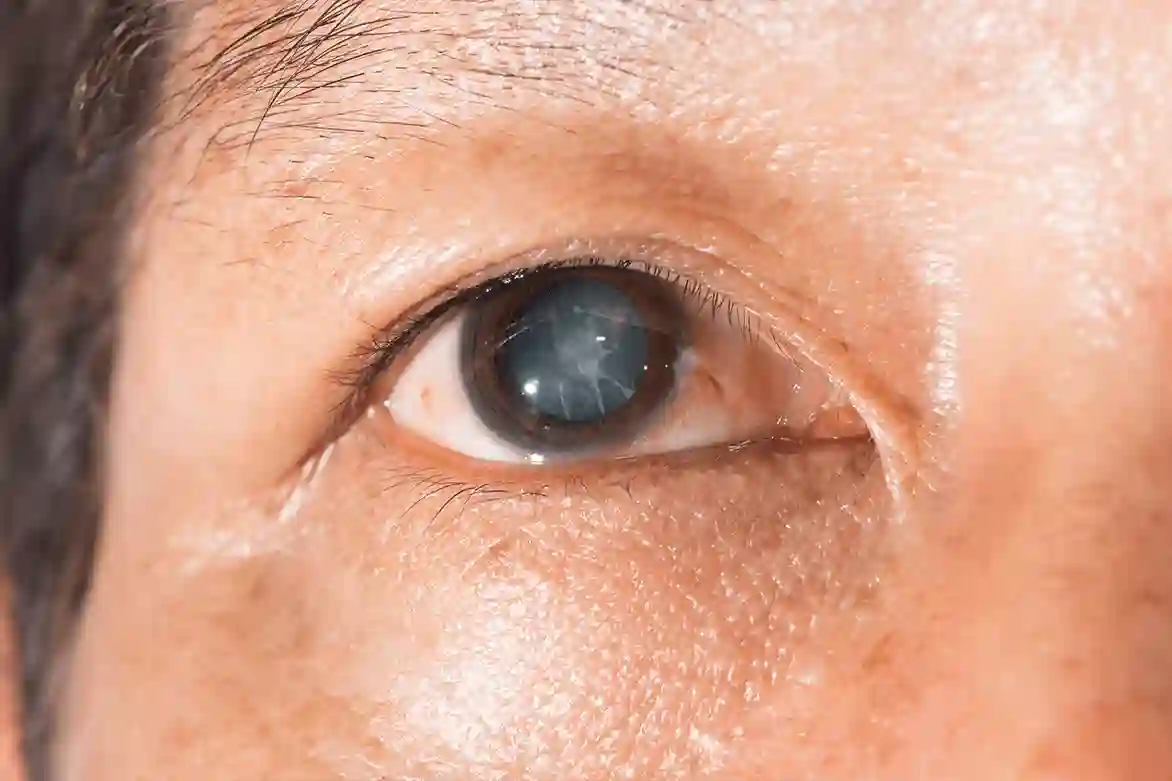
A cortical cataract is a type of age-related cataract that starts in the outer part of the lens of the eye, called the cortex. Instead of the lens staying clear like glass, white or grey “spokes” or wedge-shaped areas appear, starting near the edge and slowly growing towards the centre.
In simple terms, light entering the eye gets scattered by these cloudy wedges instead of passing cleanly to the retina. This is why people with cortical cataract often say:
- “I can see, but there is a lot of glare.”
- “Lights at night look star-shaped or streaky.”
Bottom line, the cortical cataract meaning is ‘a cloudy change in the outer layer of the lens, forming spoke-like opacities that affect how light passes through.’
Cortical Cataract Causes
We do not have one single cause, but research has identified several important cortical cataract causes:
- Ageing of the lens: With age, the proteins and fibres in the lens change and absorb more water. This swelling and structural change in the cortex can create the spoken or wedge-shaped opacities.
- Ultraviolet (UV-B) light exposure: Large population studies show that excess sunlight exposure is strongly linked to cortical cataract, more than to some other cataract types. People who work outdoors for many years without UV protection (farmers, construction workers, street vendors) have higher rates.
- Diabetes: Diabetes changes the lens metabolism and draws extra water into the lens fibres, which can speed up the development of cortical and posterior subcapsular cataracts.
- Smoking: Smoking increases the risk of all age-related cataracts, including cortical, by increasing oxidative stress on lens proteins.
- Steroid use and other factors: Long-term use of systemic or high-dose topical steroids, previous eye inflammation, trauma, and ionising radiation can all increase cataract risk, in combination with aging.
- Genetics: It is also important to remember that many people develop cortical cataract without any obvious risk factor apart from age and family genetics.
Stages of Cortical Cataract
The stages of cortical cataract describe how far the spoke-like opacities have progressed from the outer lens towards the centre. Clinically, doctors think in three broad stages:
- Early / Incipient cortical cataract: Fine, wedge-shaped opacities appear at the extreme periphery of the lens. They are not yet in the central visual axis, so vision is still fairly good, but the patient notices mild glare or halos at night.
- Progressive cortical cataract: The “spokes” become thicker and start extending more towards the centre of the pupil. Glare becomes more troublesome, contrast sensitivity falls, and reading in bright light can be difficult.
- Mature / Advanced cortical cataract: Multiple wedges meet near the centre, and a large part of the cortex is opaque. Vision can be quite blurred even in normal light, and daily tasks like reading, driving, or recognising faces become difficult.
It is common for a person to have different stages in the two eyes, and to have a mixture of cortical, nuclear or posterior subcapsular changes at the same time.
How Common Are Cortical Cataracts?
Cataract in general is very common with age; globally, cataract remains the leading cause of blindness and a major cause of moderate to severe vision impairment.
When we look specifically at cortical cataract:
- In a large cohort from the United States, about 5.4% of eyes had cortical cataract on detailed lens photographs.
- A 10-year study reported that around 22% of participants developed new cortical cataract over a decade.
- Indian and other Asian population studies show a high overall prevalence of cataract in older adults (over 50% in people aged 60+), with cortical cataract being one of the common forms, especially in some urban samples.
Symptoms of Cortical Cataract
Cortical cataract symptoms come from light being scattered by those wedge-shaped opacities in the lens. These symptoms progress slowly, which is why patients adapt without realising how much they have lost, until cataract becomes more advanced.
People describe:
- Glare and difficulty with bright light:
Headlights, sunlight on water, or oncoming vehicles at night feel very disturbing. This happens because the spokes bend and scatter light in many directions.
- Blurred or hazy vision:
Vision feels “foggy” or “milky”, especially in bright conditions. Sometimes the person sees better on cloudy days than in harsh sunlight.
- Poor contrast and depth perception:
Colours look washed out, and judging steps or kerbs becomes harder.
- Frequent change in glasses prescription:
Despite changing glasses, the overall clarity and comfort do not improve much.
Cortical Cataract Diagnosis
Diagnosing a cortical cataract is straightforward during a comprehensive eye exam.
The steps include:
- History and visual acuity test:
You describe your symptoms (glare, blurred vision, difficulty driving at night). And your distance and near vision are measured with a chart.
- Slit-lamp examination:
The doctor uses a special microscope (slit lamp) to look at the front of your eye and lens. Cortical cataract appears as white or grey wedge-shaped opacities starting in the outer cortex and extending inwards.
- Dilated lens and retinal exam:
Eye drops are used to enlarge your pupils so the doctor can examine the entire lens, retina and optic nerve. This helps rule out other causes of vision loss, such as macular degeneration or diabetic retinopathy.
Sometimes additional tests (contrast sensitivity, glare testing, retinal OCT) are done if your symptoms seem worse than what the cataract alone would explain.
Cortical Cataract Grading
When doctors talk about cortical cataract grading, they are referring to standard systems that help them describe how much of the lens is affected.
In everyday clinic language, your doctor will simply tell you that you have “early”, “moderate” or “advanced” cortical cataract, based on how much of the lens circumference is involved and whether the central visual axis is affected.
Two widely used systems are:
- LOCS III (Lens Opacities Classification System III)
It uses standard photographs taken with a slit lamp. Cortical opacity is graded on a scale (for example 0.1–5.9) by comparing the patient’s lens to reference images.
This system has good agreement between different observers and is commonly used in research and many clinics.
- AREDS grading (Age-Related Eye Disease Study):
It is used in large clinical trials to measure changes in nuclear, cortical and posterior subcapsular opacities over time. A small increase in cortical opacity score over 2 years was shown to predict more significant visual impact later.
Cortical Cataract Treatment
At present, there is no proven eye drop, vitamin or medicine that can reverse a cortical cataract once it has formed. Large reviews and guidelines continue to state that surgery is the only effective way to remove an established cataract.
Treatment is therefore planned in stages:
- Early stage / mild symptoms:
New glasses or stronger lighting help for some time. Anti-glare coatings on lenses and avoiding night driving whenever possible can reduce discomfort.
- When vision starts to interfere with daily life:
If you struggle with reading, driving, work tasks, or hobbies because of glare and blur, it can be a time to consider surgery even if the cataract does not look “very dense” from outside.
- Cataract surgery:
The cloudy lens is removed and replaced with a clear intraocular lens (IOL). Modern surgery (phacoemulsification with a small incision) is highly successful; in large series, more than 90–95% of patients achieve significantly improved vision when no major other eye disease is present.
Different IOL options (monofocal, toric for astigmatism, multifocal, etc.) can be discussed with your surgeon based on your eye and lifestyle.
So for cortical cataract treatment, the key is not rushing into surgery too early, but also not waiting until vision is severely affected or complications arise.
Risks and Complications of Cortical Cataract
The cataract itself can cause problems if very advanced (for example, making the lens swollen and causing a type of glaucoma), but this is less common nowadays because most people have surgery earlier.
The more important discussion is about cataract surgery risks, which are small but real:
- Common temporary issues: Mild pain, redness or swelling in the first days after surgery or temporary rise in eye pressure or increased light sensitivity.
- Less common but more serious risks: The infections inside the eye (endophthalmitis) are rare, but vision-threatening if not treated quickly. Or significant bleeding inside the eye with retinal detachment, especially in highly myopic eyes.
Another risk is cystoid macular oedema (swelling at the centre of the retina affecting fine vision).
- Secondary cataract (posterior capsule opacification): Months or years after surgery, the capsule holding the lens can become cloudy and blur vision again. This is easily treated with a quick outpatient laser procedure (YAG capsulotomy).
Preventive Measures for Cortical Cataract
We cannot fully prevent age-related cataract, but we can reduce some risk factors or delay progression, especially for cortical cataract:
- Protect from UV light: Please wear sunglasses that block 99–100% of UVA and UVB, especially if you work outdoors. Many population studies link high lifetime UV-B exposure with a higher chance of cortical cataract.
- Manage diabetes and other systemic diseases: Good blood sugar control, blood pressure control and regular check-ups help slow lens changes associated with diabetes.
- Avoid smoking: Please stop smoking to reduce the long-term risk of all types of age-related cataract.
- Use steroids wisely: Please only use steroid tablets or eye drops when prescribed, at the right dose and for the right duration, and have your eyes monitored if long-term steroid treatment is needed.
Conclusion
A cortical cataract is a common age-related change in the lens that starts in the outer cortex and shows up as spoke-like opacities causing glare and hazy vision. Understanding the cortical cataract meaning, its causes, stages, and grading helps you interpret what your doctor is seeing and why they advise watchful waiting or surgery at different times.
While eye drops and home remedies cannot reverse this type of cataract, modern surgery can safely restore clearer vision for most people when symptoms begin to interfere with everyday life.
The best approach is to combine regular eye checks, sensible protection (UV, diabetes control, smoking cessation) and timely surgery, so that vision remains as clear and comfortable as possible through your later years.
FAQs
Can cortical cataracts be reversed without surgery?
No, cortical cataracts cannot be reversed without surgery. You can sometimes improve comfort and function for a while with new glasses, better lighting and glare protection, but only cataract surgery can remove the cloudy lens itself.
How long does it take for a cortical cataract to form?
Cortical cataracts develop slowly over years, not days or weeks, and the speed can vary a lot from person to person.
Factors like age, UV exposure, diabetes and other health issues can influence how quickly a mild cortical change progresses to a visually significant cataract.
Can you drive with a cortical cataract?
Yes, you can drive with a cortical cataract as long as your vision meets your country’s legal driving standard and you feel safe with glare, night driving and reading road signs.
Once the stages of cortical cataract progress to the point that glare and blur interfere with safe driving, your doctor will advise limiting or stopping driving until after cataract surgery.
Can diet and lifestyle changes help prevent cortical cataracts?
Yes, diet and lifestyle changes can help reduce the possibility of cortical cataracts but cannot guarantee prevention.
A diet rich in fruits, vegetables and antioxidants, not smoking, good diabetes control and regular UV protection are all sensible measures linked with lower cataract risk in large population studies.
Can cortical cataracts affect both eyes?
Yes, cortical cataracts can affect both eyes, but not always to the same degree or at the same speed.
It is common for one eye to become more symptomatic first, even though early cortical changes are present in both lenses.
Is cortical cataract serious?
Yes, cortical cataract is serious in the sense that, if it progresses and is left untreated, it can significantly reduce vision and independence.
The encouraging part is that it is a very treatable cause of visual loss, and modern cataract surgery has a high success rate when planned and performed at the right time.
What are the stages of cortical cataract?
The stages of cortical cataract are early peripheral spokes (incipient), thicker spokes extending towards the centre (progressive), and dense opacities meeting near the centre (advanced).
What are the characteristics of a cortical cataract?
The main characteristics of a cortical cataract are white or grey wedge-shaped opacities starting in the outer cortex of the lens, arranged like spokes of a wheel.
What is the difference between a cortical and a nuclear cataract?
The difference between a cortical and a nuclear cataract is that a cortical cataract affects the outer layer (cortex) and appears as spoke-like opacities, while a nuclear cataract affects the centre (nucleus) of the lens and makes it yellow or brown and more densely cloudy.
Cortical cataracts cause more glare and problems in bright light, whereas nuclear cataracts more commonly affect distance vision and temporarily make near vision seem better in early stages.
What happens if you let cortical cataracts go untreated?
If you let cortical cataracts go untreated, vision becomes gradually more blurred and glare-prone, making reading, driving and recognising faces difficult.
In very advanced cases, cataracts can lead to severe vision loss and occasionally complications such as lens-induced glaucoma; delaying surgery also means you live longer with poor quality of life than necessary.
Do cortical cataracts require surgery?
No, cortical cataracts do not always need surgery in their early stages; many people manage well for some time with updated glasses and simple lifestyle changes.
Surgery is advised when the cataract’s impact on vision starts to interfere with daily activities or when your eye doctor sees that further delay will not be in your best interest for long-term eye health and safety.