|
Key Takeaways:
|
Optic neuritis is inflammation of the optic nerve that can blur vision, dull colors, and cause eye pain that worse with eye movement. The concern is distinguishing between routine eye strain and actual optic neuritis symptoms, as well as knowing when there’s a risk of optic nerve damage.
In this guide, you’ll learn what it is, including its symptoms, causes, diagnosis, treatment options, prevention strategies, prognosis, and risk factors.
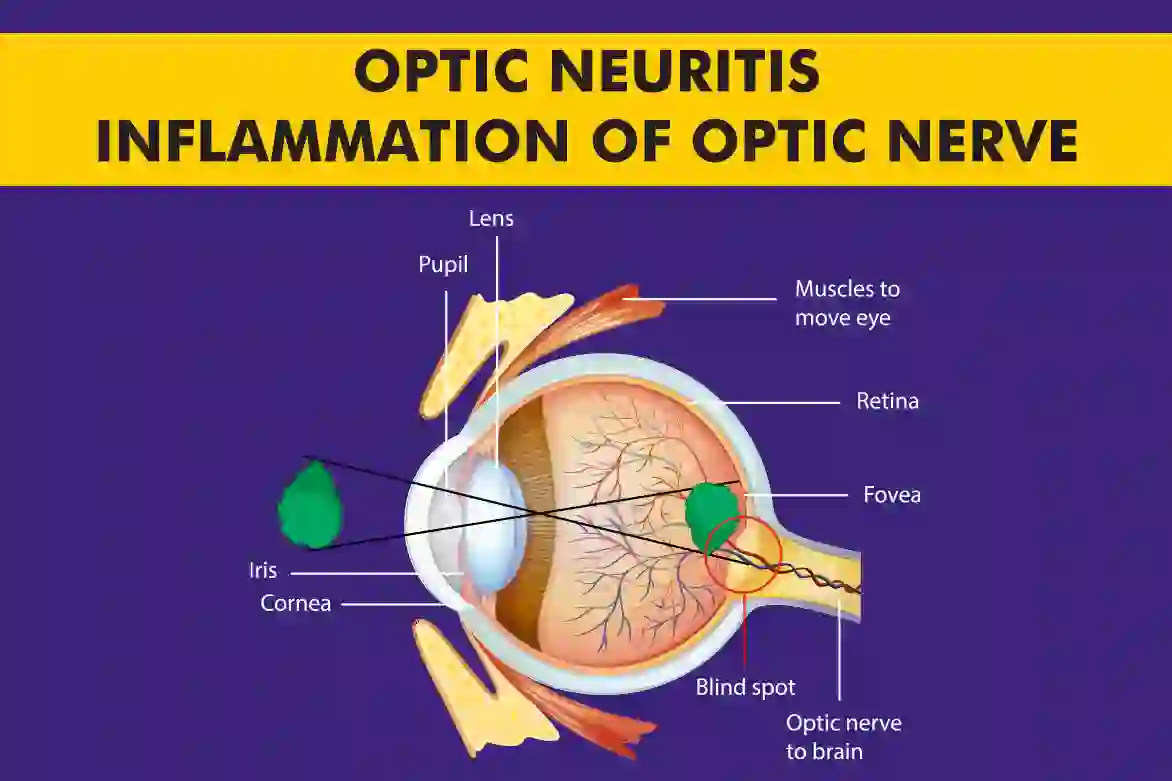
What Is Optic Neuritis (Optic Nerve Neuritis)?
Optic neuritis is inflammation of the optic nerve, the cable that carries visual signals to the brain. When it’s inflamed, vision can blur or dim, colors look washed out, and eye pain (on movement) is common. It can happen once or recur, and while any age can be affected, young adults, especially women, are seen more. Some cases link to demyelination (damage to the nerve’s myelin coating), and others are tied to infections or immune conditions.
Types of Optic Neuritis
Doctors describe three clinical patterns: typical, atypical, and pediatric and also classify by location: retrobulbar (nerve behind the eye), papillitis (swollen optic disc), and neuroretinitis (disc swelling with macular exudates).
Below are the different types of optic neuritis:
- Typical optic neuritis:
Demyelinating pattern; linked to multiple sclerosis (MS). Pain with eye movement, color dullness, and vision drop are common.
- Atypical optic neuritis:
Atypical optic neuritis doesn’t follow the classic pattern; it is due to infections, immune diseases, toxins, or antibody-mediated disorders (e.g., NMOSD/MOG). Needs tailored tests and treatment.
- Pediatric optic neuritis:
Pediatric optic neuritis occurs in children/teens, affecting both eyes, and typically follows a recent illness. Management and outlook differ from adults.
- Retrobulbar neuritis (by location):
Retrobulbar neuritis is an inflammation behind the eyeball; the optic disc looks normal early, but vision and color drop.
- Papillitis (by location):
Papillitis is a swelling of the optic disc visible on exam; vision loss and pain are present.
- Neuroretinitis (by location):
Neuroretinitis is an optic disc swelling with characteristic macular exudates (star pattern); it can follow infections or immune triggers.
What Are Optic Neuritis Causes?
Many cases are autoimmune, where your immune system attacks myelin on the optic nerve. Triggers and associations include viral illnesses, certain bacteria, toxins/medications, and systemic immune disorders. Optic neuritis is also linked with central nervous system demyelinating diseases such as multiple sclerosis (MS) and, in some patients, other antibody-mediated conditions.
Below are the most common causes of optic neuritis:
-
Multiple sclerosis and other nerve conditions
Optic neuritis may be the first sign of MS, or occur during its course. Other demyelinating conditions, like neuromyelitis optica spectrum disorder (NMOSD) and MOG-antibody disease, can also cause optic neuritis, sometimes with different patterns (e.g., more bilateral or with marked disc swelling).
Your doctor may order an MRI and blood tests to check for these associations because they affect prognosis and treatment.
-
Autoimmune conditions
Beyond MS-related demyelination, optic neuritis can appear with systemic autoimmune disease (for example, conditions that inflame blood vessels or the eye), where the immune system mistakenly targets tissue around the nerve.
Identifying an autoimmune driver helps guide therapy (such as corticosteroids or other immune-modulating medicines) and lowers the chance of relapse.
-
Infections and other causes
Viral illnesses (e.g., mumps, measles, flu) and some bacterial infections have been linked to optic neuritis, and in rarer cases, toxins or medications are implicated. When infection is suspected, doctors tailor tests and treatment to the germ involved and avoid immune-suppressing drugs until it’s safe.
What Are Optic Neuritis Symptoms?
Below are the Optic Neuritis symptoms:
- Sudden vision drop in one eye over hours to a few days (sometimes both in children).
- Eye pain, worse on movement (looking left/right or up/down).
- Colors look dull or washed out, particularly red.
- Dim or blurred vision with reduced sharpness and contrast (letters look faded).
- Patch of missing vision (central or arc-shaped “blind spot”) on Amsler/reading.
- Light sensitivity and trouble in low light.
- Symptoms that worsen with heat or exercise (some people notice temporary blur after a hot shower).
|
Note: Get urgent care if vision drops quickly, pain is severe, both eyes are affected, or symptoms come with weakness, numbness, or balance issues. |
What Are the Risk Factors of Optic Neuritis?
Below are the categories that constitutes Optic Neuritis risk factors:
- Age and sex: More common in young adults, especially women.
- Personal history: Prior episodes of optic neuritis or other inflammatory eye/nerve problems.
- Neurologic disease: Association with multiple sclerosis (MS); risk also discussed in NMOSD/MOG-antibody disorders.
- Autoimmune background: Personal or family history of autoimmune disease increases the likelihood.
- Recent illness: Viral or bacterial infections precede symptoms in some people.
Optic Neuritis Diagnosis & Tests
Below are the Optic Neuritis diagnosis & tests:
- History and eye exam: Onset/timing, pain with eye movement, and checking pupils for a relative afferent pupillary defect (RAPD).
- Vision testing: Visual acuity (distance/near), color vision and contrast tests, and visual fields to map any blind spots.
- Slit-lamp and optic nerve exam: Looking for optic disc swelling (papillitis) or a normal-appearing disc in retrobulbar neuritis.
- Optical coherence tomography (OCT): Measures nerve fiber layers and helps track recovery over time.
- MRI of brain and orbits with contrast: Looks for inflammation of the optic nerve and any demyelinating lesions that suggest MS or related conditions.
- Targeted blood tests: When indicated, will include antibodies for NMOSD (AQP4) and MOG, and screens for infections or autoimmune causes.
- Occasional lumbar puncture: If the diagnosis is unclear or to evaluate for inflammatory/infectious causes.
Optic Neuritis Treatment
Most cases improve over time, but treatment can reduce inflammation and speed recovery. For many adults with typical optic neuritis, doctors use corticosteroids, as short-course IV methylprednisolone followed by a taper in selected cases, to help vision improve faster.
If infection is suspected, treatment is tailored to the cause before using immune-suppressing medicines. Care also focuses on comfort and function while you heal: pain relief as needed, rest from heavy visual strain during the acute phase, and vision aids (better lighting, contrast settings, larger print) if reading is hard.
Your specialist will guide follow-up to monitor recovery and discuss risk of future episodes, including evaluation for optic nerve damage risk and conditions such as multiple sclerosis, NMOSD, or MOG-antibody disease. If vision does not improve as expected, or if atypical features are present, additional tests or treatments can be recommended.
Optic Neuritis Prevention
Below are the Optic Neuritis prevention tips:
- General health: Regular exercise, a balanced diet, good sleep, and stress control support immune balance.
- Infection hygiene: Wash hands, avoid touching/rubbing eyes, and manage sinus/respiratory infections promptly.
- Medical follow-up: If you have MS or another immune condition, keep neurology/ophthalmology visits and take prescribed therapy to lower relapse risk.
- Medication safety: Review new drugs or supplements with your eye specialists if you’ve had optic neuritis before.
- Eye care habits: Take screen breaks, use proper lighting, and avoid smoking to support optic nerve health.
Optic Neuritis Prognosis
Below are the Optic Neuritis prognosis:
- Average course: Many people improve over weeks to months; pain eases first, then vision, while color/contrast recover more slowly.
- Treatment effect: Steroids can speed recovery in selected cases, but don’t always change the final vision outcome.
- Long-term outlook: A subset has residual blur, low-contrast issues, or recurrent episodes; regular follow-up helps catch changes early.
- Related conditions: Your doctor will assess future MS/NMOSD/MOG risk with MRI and blood tests to guide monitoring and prevention.
Conclusion
Most people with optic neuritis improve over weeks to months, especially with timely diagnosis and care. Steroids speed recovery in selected cases, while follow-up checks help watch for related conditions. Protect your eyes by reporting new pain, color dullness, or sudden blur right away. With the right plan, vision and confidence usually return.
FAQs
What does the start of optic neuritis feel like?
The onset of optic neuritis is characterised by eye pain that worsens with movement, followed by a sudden loss of clarity or a dim, washed-out appearance in one eye.
Can optic neuritis be cured?
Optic neuritis can improve significantly, and many people recover well, but whether it can be fully cured depends on the underlying cause.
Can you live a normal life with optic neuritis?
Yes, you can live a normal life with optic neuritis by getting prompt care, following treatment, and attending check-ups; most daily activities return as vision improves.
Can optic neuritis cause blindness?
No, optic neuritis does not cause blindness. Optic neuritis can cause severe vision loss during the attack, but permanent, total blindness is uncommon with timely diagnosis and treatment.
What are the symptoms of optic neuritis?
The symptoms of optic neuritis include eye pain with movement, sudden vision loss, dull color vision (especially red), reduced contrast, and sometimes a central blurry spot.
Can the optic nerve repair itself?
No, the optic nerve cannot repair itself. The optic nerve does not regrow like skin or muscle, but inflammation can settle, and function can recover as swelling and immune activity calm down.
Can optic neuritis cause death?
No, optic neuritis does not cause death; the concern is vision loss, not death.
What can be mistaken for optic neuritis?
Conditions that can be mistaken for optic neuritis include ischemic optic neuropathy, compressive optic neuropathy, severe dry eye or migraine aura, and retinal disorders.
Can optic neuritis go away on its own?
No, optic neuritis cannot go away on its own. Getting evaluated promptly helps confirm the cause and speed recovery when treatment is needed.