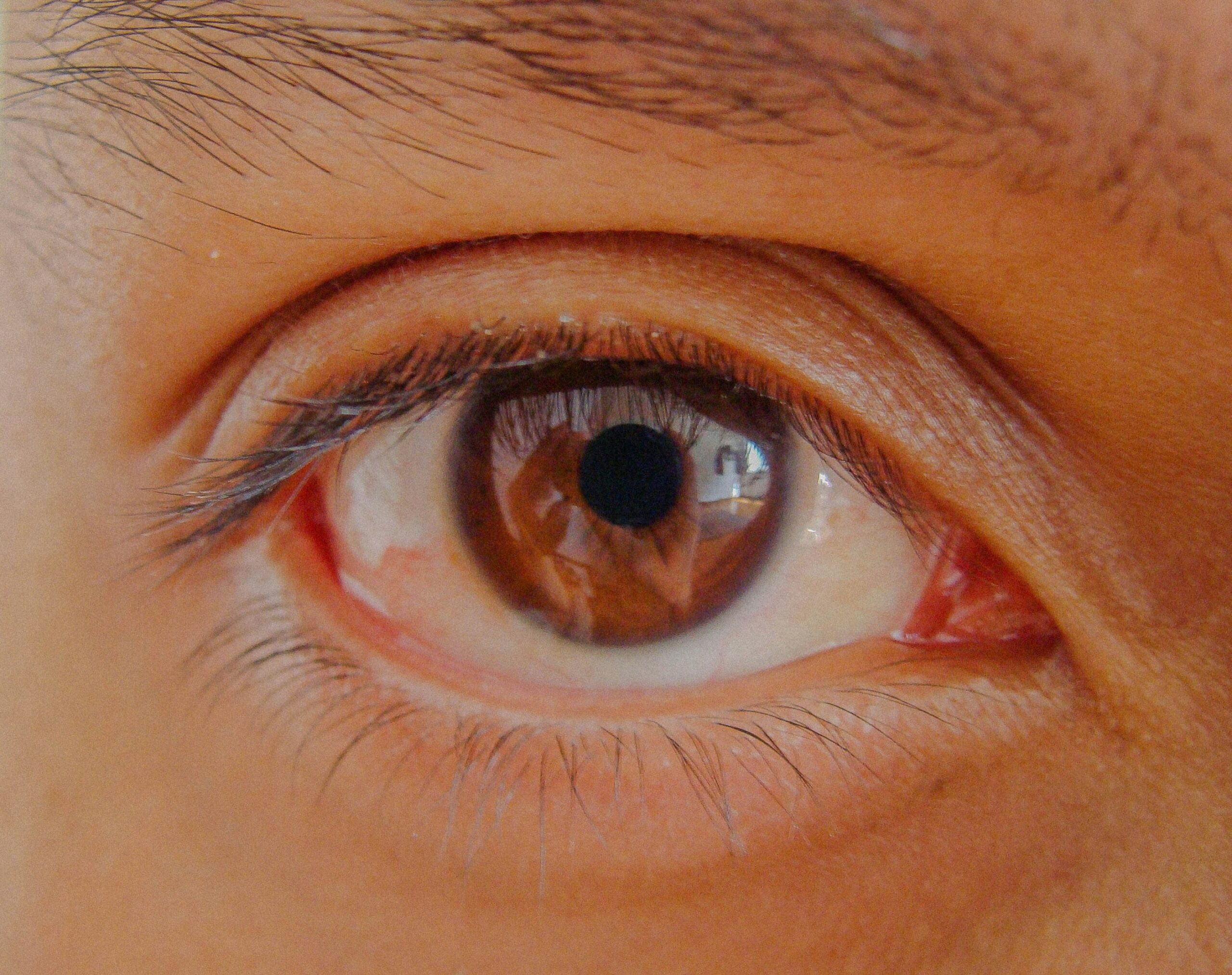
Iritis is a painful inflammation inside the eye that can make a simple “red eye” feel suddenly serious.
The problem is that many people treat it like an allergy or infection and delay the right care, even though untreated inflammation can lead to complications.
In this blog, you’ll learn the iritis meaning, what iritis disease is, common causes, symptoms, how doctors diagnose it, what iritis treatment includes, and when to see a doctor urgently.
What is Iritis? (iritis meaning)
Iritis means inflammation of the iris, the coloured ring of tissue that controls your pupil size and helps regulate how much light enters the eye.
Clinically, iritis is also called anterior uveitis (inflammation near the front of the eye).
A useful way to remember it:
- Conjunctivitis irritates the surface of the eye.
- Iritis irritates the inside/front chamber of the eye, which is why it can be more painful and more light-sensitive.
What is Iritis Disease?
“Iritis disease” isn’t a separate disease name, it’s a common way people refer to iritis as a condition.
Medically, it falls under uveitis, which means inflammation of the uveal tract (iris, ciliary body, choroid). Most uveitis cases are anterior uveitis, which is the iritis category.
- One clinical review reported the annual incidence of acute anterior uveitis at about 12 per 100,000 people. (National Library of Medicine)
- A large U.S. study reported overall uveitis incidence around 24.9 per 100,000 person-years, with prevalence around 57–58 per 100,000 in the years studied. (JAMA Ophthalmology)
Symptoms of Iritis
Iritis symptoms start suddenly and can be uncomfortable enough to make you avoid light.
- Eye pain (a deep ache, not just surface irritation)
- Sensitivity to light (photophobia)
- Redness, more around the coloured part of the eye
- Blurred vision or “hazy” vision
- Tearing (sometimes, but discharge is not the main feature)
Why does it feel different from a “normal red eye”?
Inside the eye, inflammation releases cells and proteins into the front chamber. That’s why doctors look for “cells and flare” during examinations.
Causes of Iritis
Iritis can happen on its own (idiopathic) or as part of an immune condition, infection, or injury. Many cases are idiopathic, but recurrent or severe episodes trigger a deeper cause search.
- Autoimmune/inflammatory links:
Especially HLA-B27–associated conditions (ankylosing spondylitis, reactive arthritis, psoriasis, inflammatory bowel disease).
Over ~50% of acute anterior uveitis (AAU) cases are associated with HLA-B27 in some populations.
That’s why HLA-B27 testing will be considered in recurrent cases rather than in every first episode.
- Infections inside the eye:
HSV (herpes simplex), VZV (shingles), CMV, suspected when the pattern fits (for example, certain iris changes or pressure spikes).
- Trauma:
A hit to the eye can trigger inflammation in the front chamber.
- Other systemic conditions:
Doctors may consider sarcoidosis, and other causes based on your symptoms and history.
Diagnosis of Iritis
Iritis is diagnosed mainly through a detailed eye exam, this is not something that can be reliably confirmed by symptoms alone.
- Slit-lamp exam to look for anterior chamber cells/flare, keratic precipitates, and iris changes.
- Eye pressure check (IOP) because pressure can rise in some types of uveitis and with steroid use.
- Pupil and lens assessment to look for adhesions (posterior synechiae) or early cataract changes in recurrent cases.
Iritis Treatment
The main goals of iritis treatment are:
- calm inflammation,
- reduce pain and light sensitivity,
- prevent complications (like adhesions, pressure rise, cataract).
1) Anti-inflammatory eye drops (topical corticosteroids)
Steroid drops are the core treatment for many anterior uveitis/iritis cases, and they are started and tapered under an ophthalmologist’s supervision over the course of weeks instead of days.
Steroids can raise eye pressure and (with longer use) contribute to cataract risk in some people, that’s why follow ups are important so the doctor can adjust the dosage accordingly.
2) Cycloplegic/dilating drops (pain + protection)
Cycloplegic drops relax the focusing muscle and keep the pupil moving less, which:
- Reduces pain from muscle spasm, and
- Helps prevent/break posterior synechiae (iris sticking to the lens).
3) Treat the root cause when needed
- If a viral pattern is suspected (HSV/VZV/CMV), antiviral treatment will be considered alongside inflammation control.
- If there’s a strong systemic link (like HLA-B27 inflammatory arthritis), coordinated care with a rheumatologist reduces recurrence risk and protects long-term vision.
Can Iritis Be Cured?
Many cases of acute iritis improve well with timely treatment, but “cure” depends on the cause.
- If it’s a one-time episode, it can be resolved fully. Anterior uveitis can start suddenly and symptoms last weeks, but uveitis can also cycle and recur.
- If it’s linked to an underlying inflammatory condition, it will be recurrent and needs long-term strategy.
Recurrence: what studies show?
- A study following first-episode anterior uveitis found relapse incidence 24% per person-year, and 39% had a recurrence during follow-up. (National Library of Medicine)
- A large recurrence study reported 10-year ipsilateral recurrence rates of 38.1% (idiopathic) and 43.2% (HLA-B27/inflammatory arthritis). (National Library of Medicine)
So, many people do well, but recurrence is common enough that proper diagnosis and follow-up really matter.
When to See a Doctor?
You should not “wait it out” if the symptoms fit iritis.
See an eye doctor urgently if you have:
- Red eye + pain + light sensitivity
- Blurred vision that doesn’t clear with blinking
- A history of uveitis/iritis and symptoms are returning
Seek emergency care immediately if:
- There is sudden major vision loss, severe pain, or rapidly worsening symptoms (doctors need to rule out other emergencies too).
Conclusion
Iritis is inflammation of the iris and is one of the most common forms of uveitis, causing pain, redness, and strong light sensitivity.
The challenge is that it can look like a routine red eye, but it needs a slit-lamp diagnosis and careful treatment to prevent complications like pressure rise, adhesions, and cataract changes, especially in recurrent cases.
If symptoms start suddenly, getting checked early is the simplest way to protect vision and reduce the chance that a short episode turns into a long-term problem.