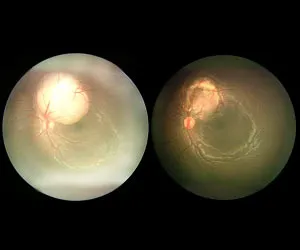
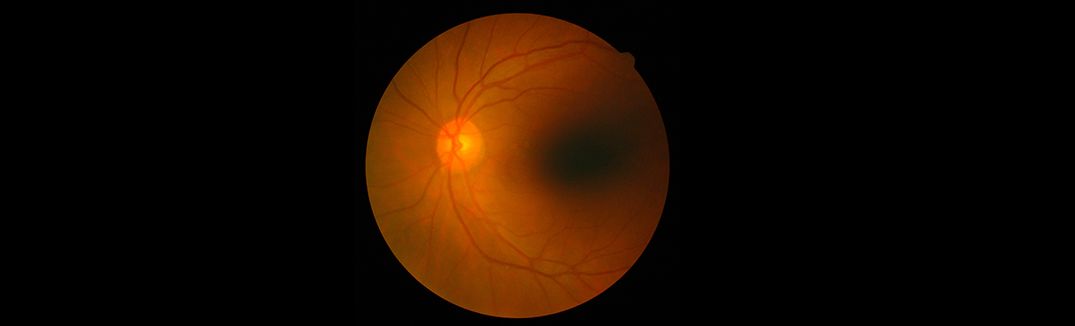
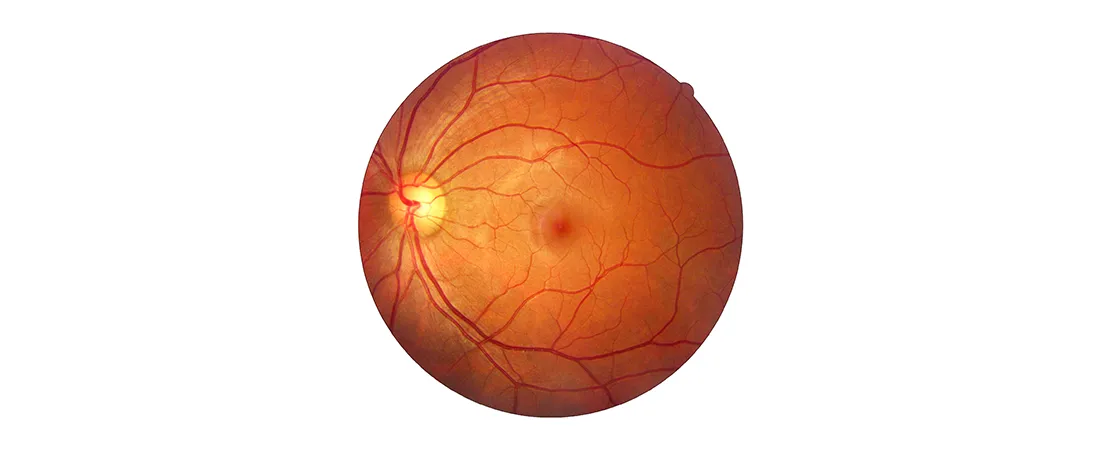
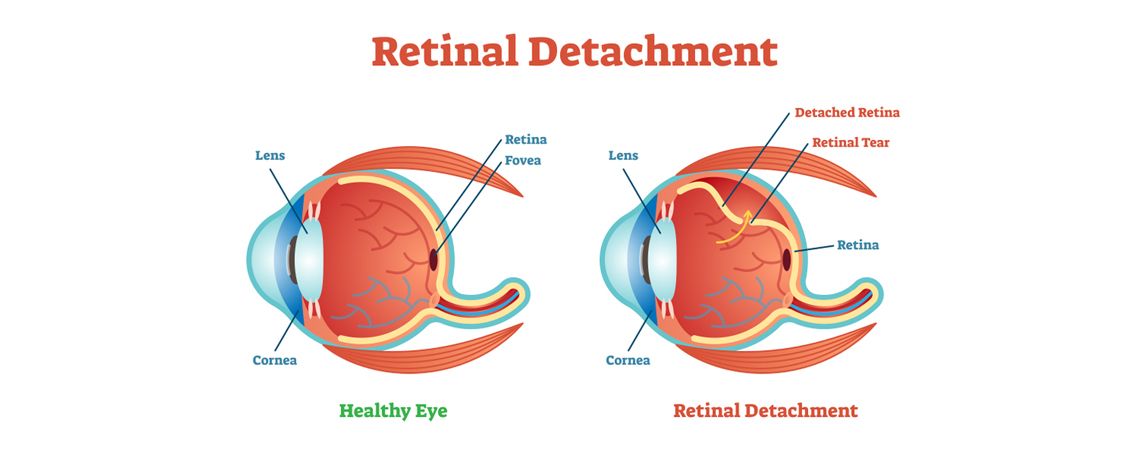
The light sensitive tissue lining the back of the eyes is known as Retina. It is responsible for converting the light rays into impulses that travel through the optic nerve to our brain, where they are interpreted as what we see as images. Vitreous gel, the clear material that fills the eyeball, is attached to the retina in the back of the eye. As we get older, the vitreous may change shape, pulling away from the retina. If the vitreous pulls a piece of the retina with it, it causes a retinal tear. Once a retinal tear occurs, vitreous fluid may seep through and lift the retina off the back wall of the eye, causing it to detach or pull away. When the tissue around the retina gets separated from it, a serious eye condition called Retinal Detachment develops. Based on the different circumstances that cause it, there are different types of Retinal Detachment that people suffer from.
Types of Retinal Detachment based on their Causes
Rhegmatogenous –
The type of Retinal detachment caused by a tear or hole in the retina is called Rhegmatogenous Retinal Detachment. It is one of the most common types, and the affected part of the retina stops working, causing you to have reduced vision. It is usually found in older people as its occurrence is in direct correlation to the aging process.
Tractional –
Commonly occurring in patients with diabetes or other such conditions, Tractional Retinal Detachment is caused by the development of scar tissues on the retinal surface. This makes the retina to detach from the back of the eye and subsequent loss of vision. It is not as common as the Rhegmatogenous type.
Exudative –
This type of Retinal Detachment occurs because of age-related macular degeneration (AMD), inflammatory disorders, injuries to the eye, or tumors in the eye. The fluid accumulation beneath the retina, in this case, is not due to any tear or hole in it. But if it is happening due to AMD, then the patient is usually in the older age bracket.
Common Symptoms of Retinal Detachment
While all the types mentioned above of Retinal Detachment are usually painless when one occurs, it does have some symptoms that precede it, such as:
- An unexpected appearance of many little specks swimming in your field of vision. These drifting specs are also known as floaters.
- Individuals also perceive flashes of light in their vision, called photopsia. This may occur in one or both of the eyes.
- Like many of the eye related issues, one of the main symptoms of retinal detachment is also blurred vision.
- The field of vision also becomes narrower as the patient’s peripheral vision is reduced and grows darker.
- In some cases, patients also see straight lines to be slightly curved.
- Retinal detachment makes a seemingly curtain-like shadow land on your field of vision.
- The patient experiences a momentary heavy feeling in the eye or eyes that are affected.
How can it be treated?
There are a number of ways that a retinal detachment can be treated. Retinal tears or holes usually require a Laser (thermal) or freezing (cryopexy). Both of these approaches can repair a tear in the retina if it is diagnosed early enough. If it is not detected early, then Retinal detachments may require surgery to return the retina to its original position. Pneumatic retinopexy is the procedure that can be used to treat retinal detachment if the tear is small and easy to close. A small gas bubble is injected into the eye (specifically into the clear, gel-like substance between the lens and the retina), where it then rises and presses against the retina, closing the tear. A laser or cryopexy can then be used to seal the tear. Another treatment method goes by the name Scleral buckle which involves surgically sewing a silicone a scleral buckle or flexible band is placed around the equator of the eye to counterbalance any force pulling the retina out of place.
This band is not visible and remains permanently attached. Laser or cryo treatment may then be necessary to seal the tear. Vitrectomy is the surgery type for retinal detachment which is used for large tears. During this, the doctor removes the vitreous (the clear, gel-like substance between the eye’s lens and retina) and replaces it with a saline solution. Depending on the complexity of the retinal detachment, various combinations of vitrectomy, buckle, laser, and gas bubbles may be used to repair the retina. Vision may take many months to improve and in some cases may never fully return.
Prevention is always better, so keep yourself updated about the condition of your eyes. People who are especially at risk of Retinal Detachment should take precautions.
At Risk Cases
- Individuals who have previously had a Retinal Detachment in one of the eyes are more likely to have it in the other eye too.
- Aging increases the chances of it as seen in cases with age-related macular degeneration. Thus, people over 50 years of age are more at risk of such detachment.
- If you have a family history of this problem, you’re more likely to have it.
- Patients who’ve had complicated eye surgeries may develop Retinal Detachment. These surgeries especially include cataract removal.
- People who have suffered from other eye diseases like uveitis or retinoschisis are more at risk. Previously suffered eye disorders make your eyes more susceptible to Retinal Detachment.
- Individuals who have an extreme case of myopia or nearsightedness also get Retinal Detachment easier than others without it.
- People whose eyes get direct contact from either sports or their jobs are also at risk. It is known that physical trauma to the eye can be a cause of detachment of the retina.
Unfortunately, some patients, particularly those with chronic retinal detachment, do not recover any vision. For this reason, it is very important to see your ophthalmologist at the first sign of trouble. It is categorized as a medical emergency because if not treated at the right time, there are no further cures or treatments to bring back your vision.
Article: Retinal Detachment Treatment – Causes & Cure
Author: Dr Saurabh Arora | Feb 16 2016 | UPDATED 02:00 IST
*The views expressed here are solely those of the author in his private capacity and do not in any way represent the views of Centre for Sight.