|
Key Takeaways:
|
Intraocular pressure (IOP) is the fluid pressure inside your eye that stays healthy when fluid production and drainage are in balance. The confusion is that pressure can be “normal” yet still risky for some people, or spike quietly and raise the chance of optic nerve damage and glaucoma .
In this blog, you’ll learn what normal intraocular pressure means, why it changes, how doctors measure it, and safe ways to manage or lower eye pressure, naturally and with treatment.
What is Intraocular Pressure?
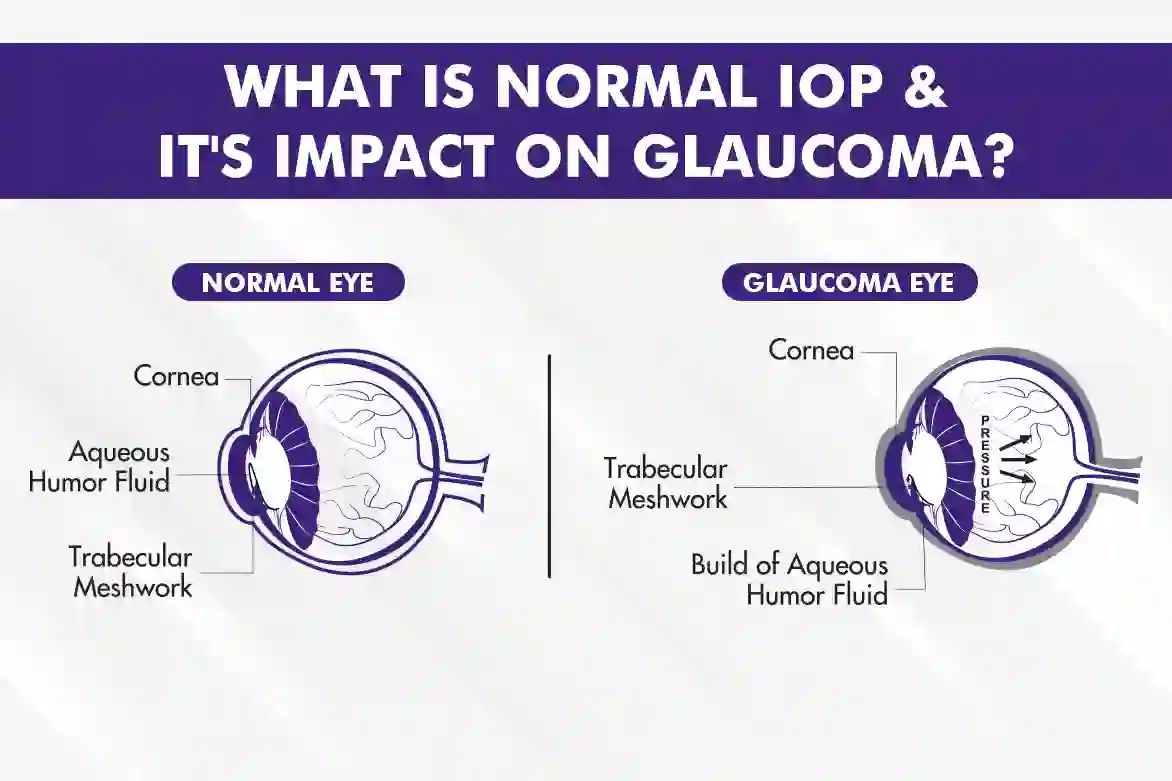
Intraocular pressure (IOP) is the fluid pressure inside your eye. Your eye makes a clear fluid (aqueous humour) and drains it through tiny channels near the cornea’s edge. When production and drainage stay in balance, pressure stays healthy; when that balance shifts, pressure can rise or fall. IOP is measured in millimetres of mercury (mmHg) during an eye exam with a test called tonometry. A “normal” reading isn’t the same for everyone; some optic nerves are sensitive even at average pressures, while others tolerate higher numbers.
That’s why doctors look at pressure and the optic nerve together before deciding on risk or treatment. Think of IOP as the eye’s “tyre pressure”: enough to keep the eye’s shape and optics stable, but not so high that it strains the optic nerve.
Regular checks help catch quiet pressure changes early, especially if you have risk factors like family history of glaucoma, high myopia, diabetes, or long-term steroid use.
Measuring Eye Pressure
A clear intraocular pressure (IOP) check begins with the right test, a sensible target range, and an understanding of factors that can skew a reading. Below is a simple breakdown you can use as-is:
Methods Used for IOP Measurement
- Goldmann applanation tonometry (GAT): The clinic gold standard. A tiny probe gently flattens the cornea after numbing drops; the force needed estimates IOP.
- Non-contact tonometry (air-puff): No drops or contact. Good for screening; high results are usually confirmed with GAT.
- Rebound tonometry: A handheld probe briefly taps the cornea and measures the rebound speed. Handy for children, community checks, and home use.
- Dynamic contour tonometry (DCT): A contoured tip matches the cornea to reduce thickness-related error; useful when corneal properties make GAT less reliable.
- Pachymetry: Measures corneal thickness so the clinician can interpret IOP more accurately.
Normal Range of Intraocular Pressure
- The clinic range is ~10–21 mmHg.
- “Normal” is not the same for everyone; some optic nerves are sensitive at average pressures (normal-tension glaucoma), while others tolerate higher numbers.
- Doctors set a target IOP for each eye based on nerve health, fields/OCT, and risk factors, not just the number on the day.
Factors Affecting Eye Pressure Readings
- Time of day & posture: IOP follows a daily rhythm ( higher in the morning) and can rise when lying flat.
- Corneal thickness & biomechanics: Thin corneas tend to underestimate, thick corneas can overestimate with some devices; pachymetry helps correct the picture.
- Technique & device: Poor fixation, squeezing lids, or repeated air-puffs can skew results; confirmation with GAT is common.
- Medications: Steroids (drops, inhalers, tablets) can raise IOP; glaucoma drops (beta-blockers, prostaglandin analogues, etc.) lower it and thus the measured value.
- Age & eye health: Ageing reduces outflow efficiency, and prior eye surgery or injury can alter true IOP and its variability.
Causes of Eye Pressure Fluctuations
IOP isn’t a fixed number. It fluctuates throughout the day as your body, habits, and health change. Most shifts are small and harmless, but bigger or frequent swings matter if you’re at risk of glaucoma.
Natural Variations in IOP
Your eyes make and drain fluid all day, so pressure naturally peaks in the morning and eases later. Simple things like blinking, rubbing the eyes, holding your breath, bending or lying flat can nudge it up for a short time. These brief changes settle on their own once you relax, sit up, and breathe normally.
Lifestyle and Environmental Factors
Daily choices can push pressure up or down for a while. Strong coffee/energy drinks, large fluid intake in one go, tight collars or ties, and heavy weight-lifting or straining can raise IOP briefly. In contrast, steady aerobic activity (such as walking or cycling), good sleep, and taking breaks from prolonged screen time support healthier patterns. Heat, dehydration, or prolonged face-down position can also alter readings.
Medical Conditions That Affect Eye Pressure
Some health issues alter how fluid leaves the eye or how the optic nerve responds to pressure. Glaucoma directly involves pressure control and optic nerve health. Diabetes and hypertension (high blood pressure) can affect the eye’s tiny vessels and fluid balance. Sleep apnea, thyroid eye disease, prior eye injury or surgery, and uveitis (eye inflammation) can also alter IOP or its swings.
|
Important Steroid medicines (eye drops, inhalers, tablets, skin creams) are not a condition but can raise eye pressure; tell your doctor about any steroid use during IOP checks. |
Normal IOP & Glaucoma Risk
Glaucoma risk isn’t determined by a single number alone. Intraocular pressure (IOP) is crucial, but so are the health of the optic nerve, blood flow, and personal risk factors. That’s why doctors look at pressure and the nerve before setting a plan.
Relationship Between Eye Pressure and Glaucoma
Higher eye pressure puts more stress on the optic nerve and raises the chance of damage. Lowering pressure, whether through drops, laser treatment, or surgery, reduces the risk and slows the progression of glaucoma in most people. Still, some eyes are more sensitive than others, so “safe” pressure is individual.
Why Normal IOP Doesn’t Always Mean No Glaucoma (Normal-Tension Glaucoma)?
Some people develop glaucoma even with pressure in the normal range; this is called normal-tension glaucoma (NTG). Factors like reduced blood flow to the optic nerve, vascular issues (e.g., migraine, sleep apnea), or a fragile nerve can play a role. In NTG, doctors aim for an even lower target IOP and watch the nerve and visual fields closely.
Risk Factors & Early Detection
If your risk is higher, regular exams catch changes early before you notice symptoms.
- Family history of glaucoma (parent or sibling)
- Age over 40 (risk rises with age)
- Ethnicity: African, Hispanic, or Asian ancestry
- High myopia (nearsightedness) or thin corneas
- Long-term steroid use (drops, inhalers, tablets)
- Diabetes, hypertension, and sleep apnea
Importance of Regular Eye Check-ups
Regular eye exams catch intraocular pressure changes and nerve damage before vision is lost.
- Age 40–60: every 1–2 years if low risk; every 12 months if any risk factor.
- Age 60+ or high risk: every 6–12 months. High risk includes family history of glaucoma, high myopia, thin corneas, diabetes, hypertension, steroid use, or African/Hispanic/Asian ancestry.
- If your doctor is monitoring pressure/nerve changes, follow a personalised plan with 3–6 month visits that include IOP, optic nerve/OCT, and visual fields.
Early Intervention & Protective Measures
Good daily habits lower risk even when pressure looks “normal.” Keep blood pressure and diabetes under control, exercise regularly, refrain from smoking, and limit heavy caffeine intake or strenuous activities (such as wearing tight collars or holding your breath during lifts).
Tell your doctor about steroid drops/inhalers/tablets (they can raise IOP), and get checked for sleep apnea if you snore or feel very sleepy. Also, make sure close family members know to have periodic eye exams. Take the prescribed eye drops exactly as directed and keep your review appointments so that small changes can be caught early.
How to Lower Eye Pressure (Lifestyle & Medical)?
Lowering intraocular pressure (IOP) starts with daily habits and, when needed, proven medical treatments. The goal is to achieve a safe target IOP for your eye and maintain it over time.
Lifestyle Changes to Help Manage IOP
- Sleep with your head slightly raised: Use an extra pillow or a wedge to reduce night-time pressure.
- Stay hydrated in small, steady amounts: Sip water throughout the day; avoid chugging large volumes at once.
- Take screen breaks and relax your eyes: Gentle blinking and short pauses reduce strain and rubbing.
- Avoid tight collars and breath-holding lifts: Loosen ties/neckwear; breathe out during effort.
Diet and Exercise Recommendations
- Eat a balanced, heart-healthy diet: Leafy greens, colourful veggies, and foods rich in antioxidants support overall eye health.
- Go easy on salt and heavy caffeine: High sodium and multiple strong coffees/energy drinks can nudge IOP up.
- Do regular aerobic exercise: Walking, cycling, or swimming most days helps overall circulation; add gentle yoga (avoid prolonged head-down poses).
Medications for Controlling IOP
- Prostaglandin analogues: Help fluid drain out of the eye.
- Beta-blockers: Reduce fluid production.
- Carbonic anhydrase inhibitors (drops or tablets): Lower production to bring pressure down.
- Alpha agonists/combination drops: May be added if one medicine isn’t enough.
Laser & Surgical Options for Pressure Control
- SLT (selective laser trabeculoplasty): Improves outflow for open-angle glaucoma, serving as a first-line or add-on option.
- Laser iridotomy: Creates a tiny opening for narrow angles/angle-closure risk.
- MIGS (minimally invasive glaucoma surgery): Micro-stents or devices to improve drainage, combined with cataract surgery.
- Trabeculectomy/drainage devices: For tougher cases needing stronger, long-term pressure control.
When Treatment Is Necessary?
Treatment is needed when IOP is above your safe target, the optic nerve shows damage, or visual fields/OCT are worsening. High-risk eyes (strong family history, very thin corneas, or signs of normal-tension glaucoma) may need earlier treatment even at “normal” pressures. Your doctor combines pressure readings, nerve health, and test results to choose the right plan and review schedule.
Conclusion
Normal intraocular pressure is a range, not a single “safe” number, and some eyes need lower targets to protect the optic nerve. Pressure can change throughout the day, so eye specialists look at IOP together with the nerve, visual fields, and OCT scans. With steady habits and the right drops, laser, or surgery, most people keep pressure in control over time. Regular check-ups are important because glaucoma damage is often silent in its early stages.
FAQs
What is the IOP full form?
The IOP full form is intraocular pressure.
What does intraocular pressure mean?
The meaning of intraocular pressure refers to the fluid pressure inside the eye, which is created by the balance of fluid production and drainage.
What is normal intraocular pressure?
The normal intraocular pressure range is about 10–21 mmHg; however, the safe target can be lower for some eyes.
Is 23 eye pressure too high?
A pressure of 23 mmHg is above the usual clinic range and is considered elevated for many people; your doctor will confirm with repeat tests and set a personal target.
What is the danger zone for eye pressure?
The danger zone for eye pressure starts when the pressure stays well above normal (>25–30 mmHg) or spikes very high (40–60+ mmHg) with pain/redness, which needs urgent care.
What is the normal intraocular pressure in the right eye?
The normal intraocular pressure range is the same for both eyes, typically ranging from 10 to 21 mmHg.
Who is most at risk for developing high eye pressure or glaucoma?
The most at risk for developing high eye pressure or glaucoma are people over 40, those with a family history of glaucoma, high myopia, thin corneas, diabetes, hypertension, or long-term steroid use.
Can screen time or digital eye strain increase intraocular pressure?
No, screen time mainly causes dryness and strain, and IOP changes are usually small or negligible for most people.
Can high IOP return even after treatment?
Yes, pressure control can drift over time; adherence to drops, follow-ups, and occasional treatment changes keeps IOP at your safe target.