|
Key Takeaways
|
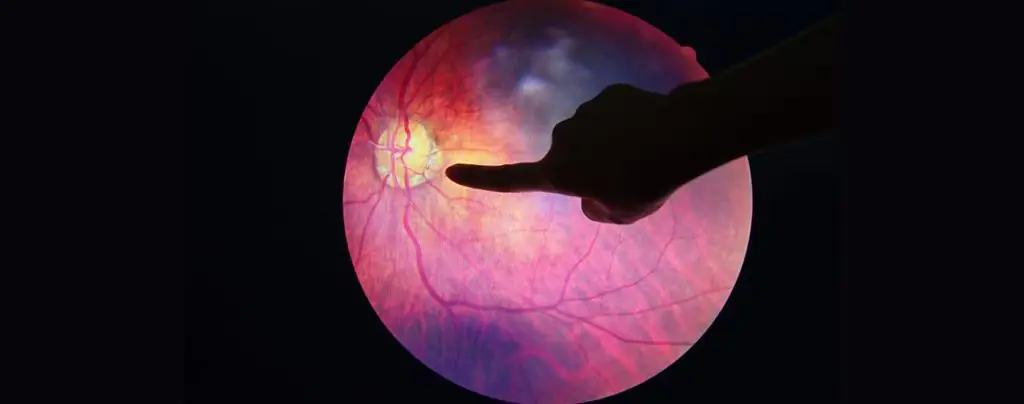
Diabetic retinopathy occurs when high blood sugar levels damage the tiny blood vessels of the retina, the light-sensitive layer at the back of the eye. Prolonged high glucose causes these vessels to swell, leak fluid, or close off. Later stages involve fragile, abnormal vessel growth, which can bleed or form scar tissue. This damage interferes with light processing, causing vision disturbances and potential permanent loss. People with type 1 or type 2 diabetes are prone to developing it.
What is Diabetic Retinopathy?
To understand diabetic retinopathy, it is important to first understand retinopathy meaning. Retinopathy refers to any disease or damage that affects the retina, which is the light-sensitive layer at the back of the eye. When the retina is damaged, vision becomes blurred, distorted, or in severe cases, permanently lost.
There are different types of retinopathy, but diabetic retinopathy is one of the most common and serious forms. Diabetic retinopathy occurs when high blood sugar levels damage the tiny blood vessels of the retina. The high blood sugar levels can restrict the movement of blood in the retina, causing the blood vessels to swell and leak. In some of the rare cases, new blood vessels can grow on the retina abnormally.
According to the National Health Portal of India (NHP India), one of the leading causes of chronic blindness includes diabetic retinopathy. Although diabetic patients are indeed at a higher risk of blindness than people without diabetes, they can also have healthy eyes given that they consult an eye specialist regularly, properly take care of their diet and medications and adopt good lifestyle practices.
If left untreated, it can cause diabetes-related vision loss, but early detection through a vision test can prevent severe damage.
Symptoms of Diabetic Retinopathy
In the early stages, diabetic retinopathy symptoms may be mild or completely absent. This is why many patients do not realise damage is occurring until it becomes advanced. As it progresses, you may experience:
- Fluctuating & Blurry vision
- Floating spots (floaters) in the field of vision
- Difficulty seeing colours clearly
- Poor night vision (Night blindness)
- Sudden or partial vision loss
If you notice these warning signs, visit a diabetic retina specialist immediately.
Diabetic Retinopathy Causes
The primary cause of diabetic retinopathy is long-term uncontrolled blood sugar levels. However, several additional factors can increase the risk:
- Duration of diabetes (risk increases after 5–10 years)
- Poor blood sugar control
- High blood pressure
- High cholesterol
- Pregnancy in diabetic women
- Smoking
Who is at Higher Risk of Diabetic Retinopathy?
Anyone with diabetes can develop diabetic retinopathy. However, the risk increases in people who:
- Have had diabetes for more than 5–10 years
- Frequently experience uncontrolled blood sugar spikes
- Have coexisting high blood pressure or high cholesterol
- Are pregnant and diabetic
- Miss regular eye checkup (screenings)
Both Type 1 and Type 2 diabetes patients are at risk. Even if vision feels normal, retinal damage may already be developing silently. This makes preventive screening extremely important.
How is Diabetic Retinopathy Diagnosed?
A comprehensive dilated eye examination is the most effective way to detect diabetic retinopathy early. During the test, the doctor may use retinal imaging, optical coherence tomography (OCT), or fluorescein angiography to examine blood vessels and detect leakage or swelling. These painless tests help identify damage before symptoms appear, allowing timely treatment and preventing irreversible vision loss.
Diabetic Retinopathy Treatment
Treatment of diabetic retinopathy is highly dependent on the stage of the disease and the presence of Diabetic Macular Edema (DME). The goal of treatment is to halt progression, reduce leakage, and prevent vision loss. Depending on the severity of the disease, there are three types of treatments, following:
- Laser therapy: In this method, high-energy laser light is used to create tiny burns in the retina. This therapy seals leaking vessels and prevents new ones from forming.
- Eye injections: In this treatment method, medications are injected directly into the vitreous gel. They block Vascular Endothelial Growth Factor (VEGF), the chemical signal responsible for stimulating abnormal vessel growth and leakage. This helps reduce swelling and control vessel growth.
- Vitreoretinal surgery: Removes blood or scar tissue when vision is severely affected. This treatment method is used in severe complications, such as non-clearing vitreous hemorrhage (blood in the eye) or tractional retinal detachment (scar tissue pulling the retina).
With timely diabetic retinopathy treatment, many patients can maintain good vision.
Prevention and Long-Term Eye Care for Diabetic Retinopathy
While diabetic retinopathy cannot always be completely prevented, its onset and progression can be significantly delayed with consistent systemic control and regular eye monitoring. People with both Type 1 and Type 2 diabetes are at risk, particularly when blood sugar levels remain uncontrolled over long periods. The risk increases further with longer duration of diabetes, pregnancy-related diabetes, smoking, high blood pressure, and elevated cholesterol levels.
Effective prevention focuses on controlling these risk factors through the following measures:
- Maintain strict blood sugar control
Consistently managing blood glucose levels is the most important step in reducing retinal damage. Follow your prescribed diabetes treatment, monitor blood sugar levels regularly, and adopt a balanced lifestyle that includes physical activity and a nutritious diet.
- Track long-term glucose control (HbA1c levels)
The glycosylated haemoglobin (HbA1c) test reflects average blood sugar levels over the past two to three months. Keeping HbA1c within the target range helps lower the risk of retinal vessel damage and allows doctors to adjust treatment early, before complications develop.
- Control blood pressure and cholesterol
High blood pressure and elevated cholesterol accelerate damage to retinal blood vessels. Managing weight, following a heart-healthy diet, and taking prescribed medications can significantly reduce the risk of vision-threatening complications.
- Quit smoking completely
Smoking worsens blood vessel damage and increases the risk of diabetic complications, including retinopathy. Quitting smoking improves overall circulation and supports better eye and systemic health.
- Schedule regular comprehensive eye examinations
Since diabetic retinopathy often develops without symptoms in its early stages, annual dilated eye exams are essential, even if vision feels normal. Early retinal changes can be detected and treated before they lead to irreversible vision loss.
By combining disciplined diabetes management with proactive eye care, individuals with diabetes can significantly reduce the risk of severe diabetic retinopathy and protect their vision over the long term.
Conclusion
Diabetic retinopathy is often called a ‘silent threat’ because symptoms appear late. Regular screening, strict blood sugar control, and timely medical care remain the most effective strategies to safeguard long-term vision. Book an appointment at Centre for Sight to ensure your eyes are examined and managed by experienced specialists.
FAQs:
Effective Treatment Approaches for Diabetic Retinopathy?
Effective treatment for Diabetic Retinopathy focuses on controlling blood sugar, blood pressure, and cholesterol. Medical interventions include laser therapy, anti-VEGF injections, and vitrectomy are used for advanced cases. Regular eye exams, lifestyle modifications, and timely management of diabetes-related complications are crucial to prevent vision loss and slow disease progression.
How do you treat diabetic retinopathy?
Control diabetes, manage blood pressure, undergo laser therapy or anti-VEGF injections, and schedule regular check-ups with an ophthalmologist.
What are the 4 stages of diabetic retinopathy?
Mild nonproliferative, moderate nonproliferative, severe nonproliferative, and proliferative retinopathy are the 4 stages of diabetic retinopathy, and each represents increasing severity of retinal damage.
What are three symptoms of diabetic retinopathy?
Blurred vision, floaters, and vision loss are common symptoms.
Does diabetic retinopathy go away?
No, it can be managed but not completely cured.
What triggers diabetic retinopathy?
Poor blood sugar control, hypertension, and long-term diabetes exposure.